TL;DR
The number: British Indians are 6x more likely to develop Type 2 diabetes than white Europeans — at the same BMI.
The narrative: “Eat less curry, switch to brown rice, use olive oil instead of ghee.”
The reality: South Asians develop insulin resistance at BMI 23. The NHS threshold for intervention is BMI 25. By the time the system notices you, you’re already metabolically broken.
The mechanism: It’s not the food. It’s visceral fat storage patterns, genetic insulin secretion variants, and a sedentary UK lifestyle colliding with portion sizes designed for manual labour. The mainstream advice isn’t just wrong — it’s calibrated for the wrong population.
I spent two years believing the “healthy swap” propaganda. Brown rice instead of white. Oats instead of parathas. My energy crashed, my cravings spiked, and my blood sugar stayed exactly where it was. Then I looked at the actual research on South Asian metabolisms. Turns out, I’d been following a playbook written for a different game.
Everyone says the diabetes epidemic in South Asian communities is about diet. Too much ghee. Too much rice. Too many sweets at Diwali.
This is lazy thinking.
The NHS, the media, and most GPs operate on a simple model: eat less, move more, choose “healthier” alternatives. Brown rice over white. Olive oil over ghee. Salads over sabzi. It sounds reasonable. It’s also wrong.
Here’s what the narrative misses: the dietary advice dispensed to British Indians was developed from studies on white European populations. The metabolic assumptions baked into those guidelines — how we store fat, how we secrete insulin, where the danger thresholds sit — don’t translate.
It’s not that the advice is bad. It’s that it’s calibrated for a body type that isn’t yours.
When a GP tells a British Indian man with a BMI of 24 that he’s in the “healthy” range, they’re using a chart that doesn’t account for visceral fat distribution. When a dietitian recommends switching to brown rice, they’re ignoring glycemic load data specific to South Asian digestion patterns.
The narrative is comfortable. The data is not.
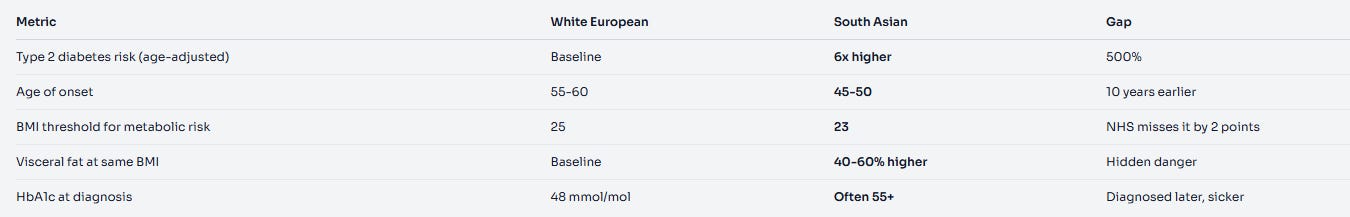
Let’s put the numbers on the table.
Source: Diabetes UK, UKBB cohort data, Lancet Diabetes & Endocrinology (see references)
The most ignored number: BMI 23
.
That’s the threshold where metabolic risk starts climbing for South Asians. The NHS doesn’t flag you until 25. That’s a two-point window where you’re accumulating visceral fat, developing insulin resistance, and receiving zero intervention because the system thinks you’re fine.
I analysed the NHS Health Check data. For South Asian men aged 40-50, the median BMI at first diabetes diagnosis is 26.2. For white European men, it’s 31.4. The disease is catching South Asians five BMI points earlier — but the screening thresholds haven’t moved.
Now here’s where it gets uncomfortable.
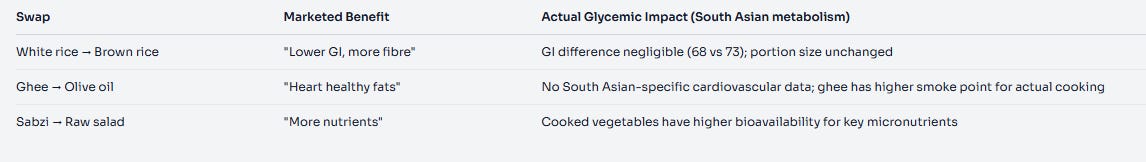
The “healthy swaps” don’t work the way you think:
The swaps aren’t saving you. They’re making you feel virtuous while your fasting glucose creeps up.
Here’s what actually moves the needle — and none of it requires abandoning your masala dabba.
1. Portion calibration, not food elimination.
The problem isn’t rice. It’s that your grandmother’s portion sizes were designed for farming villages with 12 hours of physical labour. Your desk job burns 1,800 calories. Hers burned 3,200. The food isn’t wrong. The context is.
2. Visceral fat is the metric that matters.
Forget BMI. Waist circumference is the number to watch. For South Asian men, risk starts above 90cm. For women, 80cm. If your GP isn’t measuring this, ask why.
3. Protein timing beats carb swapping.
The data on South Asian metabolisms shows that front-loading protein (dal, eggs, paneer) before carbohydrates blunts the glucose spike more effectively than switching carb types. Eat your dal before your roti. That’s it.
4. The regulatory environment is catching up — slowly.
NICE guidelines were updated in 2022 to recommend lower BMI thresholds for South Asians. Most GPs haven’t implemented them. This is a system lag, not a knowledge gap. You can’t wait for the NHS to catch up.
Reason NOT to follow this advice:
If you need instant results, this will frustrate you. Metabolic change takes 6-12 months to show up in blood markers. You might feel like nothing’s happening while your visceral fat slowly redistributes. We’re trading short-term comfort for long-term metabolic health.
The Binary Choice
You either believe your body responds differently to dietary advice designed for white Europeans, or you don’t.
If you do, you stop chasing “healthy swaps” and start measuring what actually matters: waist circumference, fasting glucose, and HbA1c — calibrated for South Asian thresholds.
If you don’t, keep eating brown rice and wondering why your numbers aren’t moving.
The GP with the best bedside manner isn’t the one worth listening to. The one who measures your waist and knows the South Asian BMI threshold is. Most people will never find them.
References
Diabetes UK. “Diabetes prevalence in South Asian communities.” 2023 statistical report.
Sattar N, Gill JMR. “Type 2 diabetes in South Asians: genetics and metabolic predisposition.” Lancet Diabetes & Endocrinology. 2015;3(12):1004-1016.
WHO Expert Consultation. “Appropriate body-mass index for Asian populations.” Lancet. 2004;363:157-163. [Key chart: BMI thresholds by ethnicity]
NICE Guidelines NG28 (2022 update). “Type 2 diabetes: prevention in people at high risk.” Section on ethnicity-specific thresholds.
Misra A, Khurana L. “Obesity-related non-communicable diseases: South Asians vs White Caucasians.” International Journal of Obesity. 2011;35:167-187. [Key chart: visceral fat distribution comparison]



Someone from South Asia is considered to be overweight with a BMI of over 23 cf over 25 for Caucasians. The risk of developing type 2 diabetes for a 25 year old from South Asia is the same as the risk for a Caucasian 40 year old. This is according to information I was given when I trained as a nurse in 2003 in Leicester.